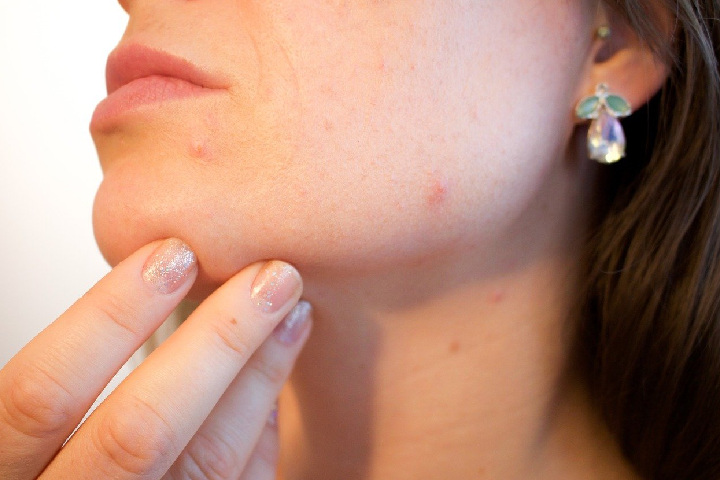
Skin lesions are a bit of the skin that has an abnormal development or appearance compared to the skin on all sides. Two types of skin lesions exist: primary and secondary. Primary skin lesions are unusual skin conditions current at birth or acquired over an individual’s lifetime.
Secondary skin lesions are the result of painful or manipulated primary skin lesions. For example, if somebody scratches a mole until it bleeds, the resulting lesion, a crust, is presently a secondary skin lesion.
Table of Contents
1. What Causes Skin Lesions?
A systemic infection (an infection that happens throughout your body), such as chickenpox or shingles, can cause skin lesions everywhere on your body. MRSA and cellulitis are two possibly life-threatening infections that involve skin lesions.

Some skin lesions are genetic, such as warps and freckles. Moles are lesions that exist at the time of birth. Others can be the outcome of a sensitive reaction, such as allergic eczema and contact dermatitis. A few conditions, like poor circulation or diabetes, cause skin sensitivity that can lead to lesions.
2. Identifying Primary and Secondary Skin Lesions
Primary skin lesions are present at the beginning of a disease. In contrast, secondary skin lesions outcome from changes over time caused by disease progression, control (scratching, picking, rubbing), or treatment. These 2 kinds of skin lesions can be differentiated as follows:
a. Primary Lesions
- Bulla — a vesicle more prominent than 5 mm in width
- Cyst — an elevated, circumscribed zone of the skin filled with fluid or semisolid liquid
- Macule — a flat, circumscribed zone; can be brown, red, white, or tan.
- Nodule — an elevated, firm, circumscribed, and a palpable area large than 5 mm in diameter; can involve all skin layers
- Papule — and the elevated, palpable, firm, circumscribed area usually less than 5 mm in width.
- Plaque — an elevated, flat-topped, firm, uneven, superficial papule greater than 2 cm in diameter; spots can coalesce to shape plaques
- Pustule — an elevated, superficial zone that is similar to a vesicle but filled with pus
- Vesicle — an elevated, circumscribed, superficial, fluid-filled blister less than 5 mm in diameter
Wheal — and elevated, irregularly shaped area of cutaneous Edema; wheals are solid, transient, and alterable, with a variable diameter; can be red, pale pink, or white.
b. Secondary Lesions
- Crust — A marginally elevated area of variable size; comprises of dried serum, blood, or purulent exudate.
- Excoriation — Linear scratches that might be denuded
- Lichenification — Rough, thickened epidermis; accentuated skin markings caused by scouring or scratching (e.g., chronic eczema and lichen simplex)
- Scale — Heaped-up keratinized cells; flakey exfoliation; irregular; thick or thin; dry or oily; variable size; can be white or tan.
3. When Should a Skin Lesion Be Removed?
Skin lesions that have no indications of being cancerous don’t need to be eliminated. If a skin tag, birthmark or other lesion is causing you significant issues though, for instance, it’s catching on dressing, you may prefer to have it eliminated.

You may also choose you to need a skin lesion eliminated if you’re unhappy with how it looks. But if you’re having it destroyed solely for cosmetic reasons, you’ll generally need to pay to have it done privately. It’s also important to realize that many of the procedures are likely to leave a scar.
Your primary care physicians will do their best to keep the spot to a minimum, but it may end up annoying you almost as much as the original lesion.
4. How are Skin Lesions Removed?
a. Complete Excision (Excision Biopsy)
This is a kind of skin biopsy, in which the entire skin lesion is cut out and removed. It’s the standard method to remove a lesion where there is any possibility that it might be cancerous. You’ll typically have a local anaesthetic before a skin biopsy, which will block any suffering.
Your primary care physician will then use a surgical blade to eliminate the whole lesion, plus a margin of ‘usual’ skin throughout the edge.
Your doctor may use sticky strips or a unique type of glue to close smaller wounds or stitches for more significant injuries. They’ll then apply a plaster to cover the injury.
b. Laser Therapy
Your doctor may recommend using treatment with lasers if you have a wart, a dermatofibroma or an actinic keratosis patch on your lips.
c. Light Therapy (Photodynamic Therapy)
This is a technique wherein a special light is used to activate a chemical applied to your lesion to destroy it. Your doctor may propose light therapy if you have actinic keratosis.
5. Which Surgical Procedure Eliminates Superficial Skin Lesions With Scraping?
Everyone with a mole, skin tag or moles always needs to know how they can get rid of them. But some people want to go through any surgical procedure that is truly invasive. So which surgical procedure eliminates superficial skin lesions with scraping?
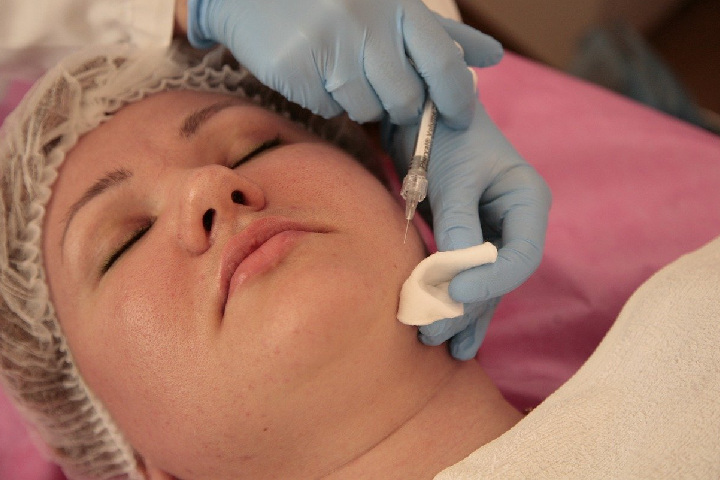
Curettage, a clinical term, is the surgical procedure that employs scraping to get rid of superficial skin lesions. In dermatological terms, it is called curettage and cautery, which is a form of electrosurgery. This procedure is finished using a curette, an instrument that looks much like a little spoon but with a truly keen edge.
The proses are so minimally invasive; it is usually done in a doctor’s office, with you as an out-patient. And it doesn’t take a long time; you can be in and out to attend to different things on your to-do list.
The Risks Involved in Curettage
There is consistently the risk of the mark with curettage. This is because the curette has to obtain all bits of the lesion. That move could quit a slight scar at the spot.
Usually, the scars are not ugly because the lesions are little, to start with. Your dermatologist can control them so that their appearance would be barely there.
However, a few people respond differently to the healing process. While scars happen from this procedure tends to be very little, theirs could be enormous and raised, instead of flat or depressed.
These types of scars have their treatment to get rid of them; however, the thick skin from them may remain. But you could use creams or lotions.
Another class of potential risks associated with curettage and cautery is damage to the nerves. Eliminating a lesion from a skin area with an extensive and intricate network of nerves could permanently or temporarily damage a few nerves.
6. How to Get Rid of Yourself?
a. Here is a Surefire Yet Effortless Way to Get Rid Yourself
Take a wad of cotton wool and immerse it in apple cider vinegar. Spot it over the lesion and cover it with a bandage. Leave the covering on for about 15 minutes, then take it off. Repeat this process every day for about 12 to 15 days.
Apple cider vinegar is most acidic, so its acid substance will weaken the tissues holding the lesion in place. This will include origin it to fall.
But before you take off on this process, ensure the lesion is started. Be sure to examine with your doctor so that you don’t touch a malignant lesion and compound the issue.
b. How to Care of the Wound After the Process
Following the procedure and the clothing of the wound, there are home consideration tips for caring for the injury. When the anaesthetic dresses off, there will be some distress, but that shouldn’t panic you. It is all part of the procedure.
c. How Do You Retain the Wound From Becoming Infected?
To Keep the Wound From Getting Infected and to Speed Up Healing:
- Take some pain killers as recommended, to ease off the pain.
- Keep from putting force on the wound and its surrounding zone.
- Leave the clothing on the wound for as your doctor guides.
- Let the wound remain dried for about 2 days or as a guide. After that time, you can wash and dry it delicately.
- If it begins to bleed for any reason, gently apply some force on it using a clean cloth for about 20 to 25 minutes. And if it continues bleeding, see a doctor as quickly as possible.
- If the open wound or the area on all sides, it becomes painful and red, it could be infected. See a doctor immediately.